The war against Covid has been underway for around two years now, far longer than many of us would have ever thought and with no sign of a sudden disappearing act just yet. So what is available for patients with Covid19 in the world, what is eligible for UK NHS use, and why aren’t the treatments readily available for all patients ill with coronavirus?
The Need For Covid19 Treatments
Covid19 struck as an unforeseen pandemic at the end of 2019, coming into full force by March 2020 in many countries worldwide. We’ve heard the word “unprecedented” more in the last two years than we would otherwise have in a lifetime. The toll thus far has been tremendous and heartbreaking, and the knock-on effects of this pandemic have spread wide and deep.
Fortunately, the likes of vaccinations can help to reduce the severity of many cases, while masks and distancing can help to reduce the spread to a degree. Unfortunately, too many still succumb to moderate, severe or fatal infection, and while the elderly or those with underlying conditions are more vulnerable, Covid19 doesn’t discriminate and can potentially severely affect anyone.
There have been various treatments touted and researched during the pandemic, many of which have been found to be ineffective. Fortunately, some newer treatments have shown more promise for helping those hospitalised with covid. Recent developments have also to led to a new wave of treatment designed for at-home use by high-risk infected individuals.
Types Of Covid Prophylaxis & Treatments
Perhaps the biggest change in our arsenal has been with the introduction of vaccines. The format, how they work and their effectiveness varies across brands, and the picture gets muddier still when considering immunosuppressed individuals or new Covid variants.
Treatments for coronavirus are not a replacement for vaccines. Vaccines aim to provide a baseline of immunity across several months. Treatments, like those below, are typically for short-term use with more immediate benefit without “teaching” your body any response to protect it from infection in the months aheads.
There are a few newer treatments for COVID19 patients at greater risk of severe illness or death. The focus on some are for avoiding hospitalisation, with treatment to be given at the onset of symptoms to hopefully prevent serious illness. Some are given at home, others require a nurse. There are also treatment for those hospitalised with COVID19 reduce the risk of severity and fatality.
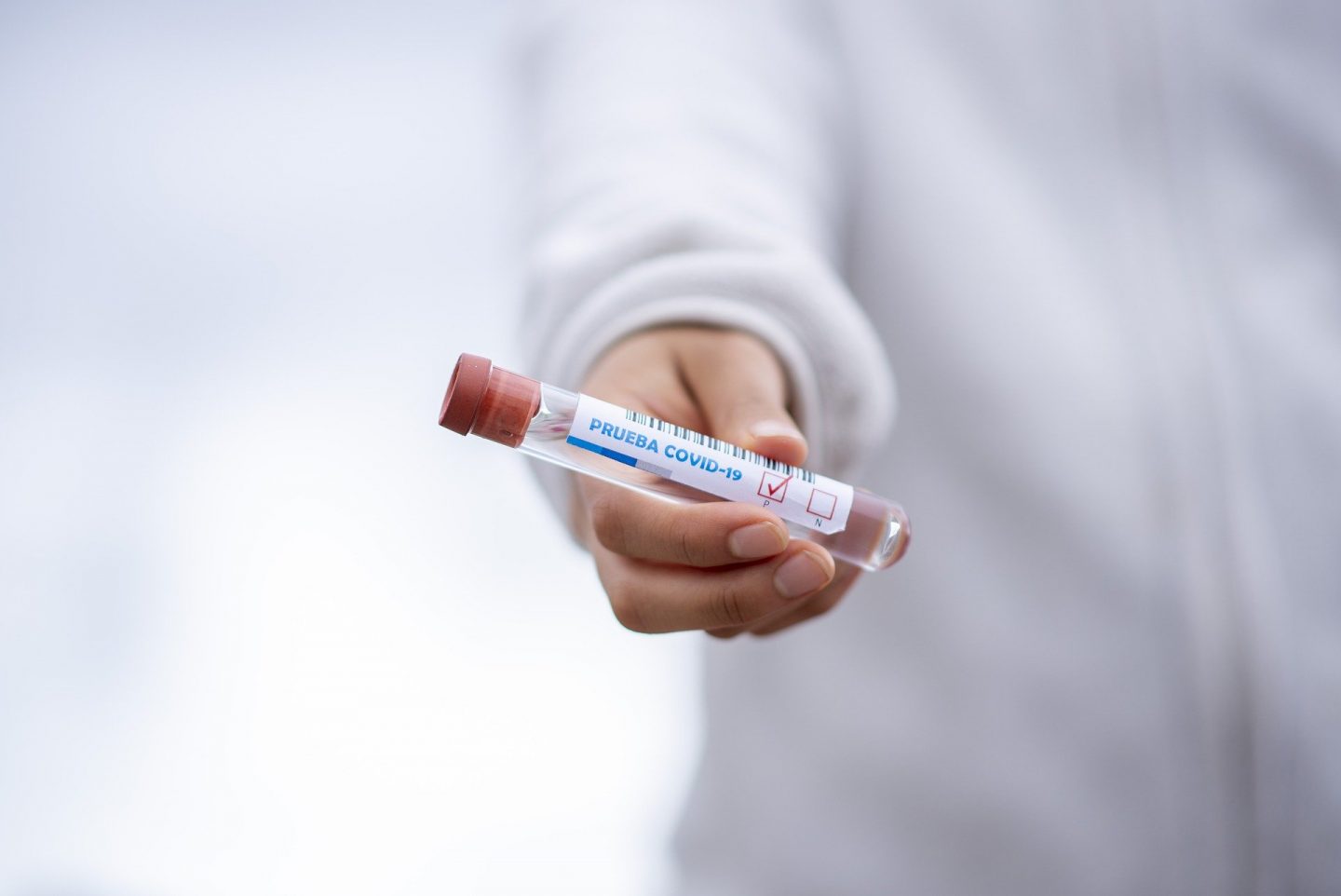
Countries will have their own directives and restrictions for who is eligible for different treatments. The UK’s NHS website provides a list of examples of pre-existing conditions that could class someone as being at higher risk of severe illness with COVID-19. This includes the likes of : autoimmune or inflammatory conditions, immunosuppressed or on immunosuppressants, HIV or Aids, certain types of cancer, Down’s syndrome, had an organ transplant, conditions affecting the brain or nerves, recent chemo or radiotherapy, and so on.
Treatments as of January 2022 are for different purposes, typically for those that are clinically vulnerable (CV) or clinically extremely vulnerable (CEV). Treatment types loosely fall into these categories :
- Treatment that aims to prevent someone developing Covid in the first instance if they’re high-risk and have been exposed to the virus : REGEN-COV/Ronapreve (Regeneron).
- Treatments for at-home use for high-risk COVID19 infected individuals that aim to prevent hospitalisation, serious illness or death : Paxlovid (Pfizer) and Molnupiravir (Ridgeback Biotherapeutics and Merck Sharp & Dohme).
- Treatments for those with mild to moderate coronavirus who’re at risk of severe illness to try to prevent worsening decline or fatality : Tocilizumab (Hoffmann-La Roche and Chugai) and Ronapreve (Roche) and Remdisivir (Gilead Sciences) and Sotrovimab (GSK & Air Biotechnology).
Antivirals vs Monoclonal Antibody Treatment
Broadly speaking, many of the medications currently available here fall loosely into antiviral or monoclonal antibody categories. Antivirals are typically active for just a few days, while monoclonal antibodies could protect an individual for a month or two after administration.
I won’t bore you with thorough details on the difference between the two, but if you’re interested in knowing which is which, then here is a brief recap. It’s worth noting that while I’ve included Remdisivir here, I’ve done so because it’s had a decent amount of media attention, though it has recently lost favour as a potential treatment.
- Paxlovid – Antiviral
- Molnupiravir – Antiviral
- Remdisivir – Antiviral
- REGEN-COV / Ronapreve – Monoclonal Antibody
- Tocilizumab – Monoclonal Antibody
- Ronapreve – Monoclonal Antibody
- Sotrovimab – Monoclonal Antibody
A Closer Look At Current Covid19 Treatments
There are a number of caveats with current treatments, not just in terms of trial limitations and supply issues, but also in how they appear less effective against the newer Omicron variant of late 2021.
Let’s take a quick look at the different types of treatments getting authorised and hopefully being put to use by January 2022.
Paxlovid (Pfizer) – Antiviral
Pfizer’s Paxlovid is available via prescription and should be used as soon as possible following a Covid19 diagnosis, preferably within 5 days of symptoms starting. This is a pill format to be taken orally at home twice a day for five days,
When taken within 3 days of symptom onset by individuals at high risk of serious illness from Covid, Paxlovid was found to be 89% effective. This dropped marginally to 88% in the first five days of symptom onset.
This medication could see a reduction in hospitalisation or death by nearly 90%. Initial findings suggested “the efficacy is high” and “the side-effects are low”, according to Dr Poland from the Mayo Clinic.
This was the first pill given emergency authorisation for at-home use in the US. On December 22nd 2021, the Food and Drug Administration granted use of Paxlovid in adults and children aged 12 and over at higher risk of hospitalisation who test positive for Covid19 and are symptomatic.
Stock availability is a challenge. Pfizer, as of December 2021, appears to have 180,000 courses of treatment available worldwide. Approximately 60,000 to 70,000 are for the States, with the US Government having agreed to buy enough Paxlovid for treating 10 million people.
The UK had initially purchased 250,000 courses, though it’s not known exactly how many they actually have to be able to give to patients. In December 2021, they agreed to purchase a further 2.5 million courses following the drug’s approval. It appears that Paxlovid in the UK will be made available via “70 new hospital clinics”, referred to as NHS Covid medicine delivery units, and treatment will then be sent to the home of the eligible infected patients.
Pfizer notes that they’re on track for producing 80 million courses for use globally in 2022, with contracts to supply the UK, US, Australia and other countries.
Ronapreve (Roche) – Monoclonal Antibody
Ronapreve is a monoclonal antibody developed by Roche. It’s a liquid format that requires refrigeration, which is then given by injection or infusion by a nurse or doctor. It’s designed to both treat and prevent acute Covid-19 infection, but it’s not a replacement for a vaccine despite some temporary prophylactic properties.
Ronapreve contains the active substances imdevimab and casirivimab. It works by attaching to the “spike protein” on the surface of the coronavirus, preventing the virus from entering cells and hopefully helping the body to overcome the infection to allow for faster recovery.
The COV-2067 study looked at Covid-19 patients who didn’t require oxygen but who were at increased risk of serious illness. Of those treated with Ronapreve, 0.9% of patients (11 out of 1,192) were hospitalised or died within 29 days of treatment, compared to 3.4% (40 out of 1193) in the placebo group.
Molnupiravir (Merck & Ridgeback) – Antiviral
Molnupiravir (Lagevrio) was developed by Merck Sharp & Dohme (MSD) and Ridgeback Biotherapeutics. It’s a capsule format that is taken orally, for use in those those who’ve tested positive for Covid19 but haven’t been hospitalised. It works through the introduction of errors to the virus’ genetic code, helping to prevent further replication and thus keep virus levels low in the hopes of reducing the disease severity.
The course involves four 200mg capsules taken orally every 12 hours for 5 days. It’s typically for at-home use and is only authorised for patients over 18 years of age. It’s designed for non-hospitalised patients with a mild to moderate Covid who’re at high risk of it progressing to severe illness or hospitalisation. In the UK, it’s authorised in people who have mild to moderate Covid and at increased risk of severe illness.
The MOVe-OUT study was used in support of of the treatment’s authorisation. Out of 709 patients who received molnupiravir, 6.8% were hospitalised or sadly died within 29 days of follow-up, compared to 9.7% of 699 patients who received a placebo.
A press release from the company claimed their Molnupiravir antiviral reduced the risk of hospitalisation or death in by roughly 50%.
The highest risk patients in the UK should be able to access Molnupiravir from 16th December 2021 onwards but stocks are very low worldwide. The UK increased their order to a total of 2.3 million courses, though it’s unknown when those will arrive and be available for use.
Sotrovimab (GSK and Vir Biotechnology) – Monoclonal Antibody
Sotrovimab (Xevudy) is a neutralising monocolonal antibody requiring an intravenous infusion (IV). It’s made by GSK and Air Biotechnology, and it works by binding to the spike protein, preventing it from entering cells and further replicating. It’s for people with mild to moderate Covid19 who’re at risk of severe illness.
This is one treatment that data presently suggests may be most effective against the Omicron variant where others are perhaps not as successful.
This is a 500mg dose administered via intravenous infusion over 30 minutes. Only one dose is required, but it appears to continue working in the body and helps to prevent reinfection for at least a month.
Clinical trial data suggests a single dose of Sotrovimab reduced the risk of hospitalisation nd deal in high risk adults experiencing symptomatic Covid19 by 79%.
It appears the most effective when administered in the early stages of infection and so it’s recommended to be used as soon as possible, preferably within 5 days of symptoms starting.
Sotrovimab was authorised by the MHRA in December 2021 for UK use.
Remdisivir (Gilead Sciences) – Antiviral
Remdisivir is an expensive experimental antiviral that was one of the first treatments touted for Covid19. It’s sold under the brand name Veklury and is given by injection into a vein. It was previously used in 2014 to treat Ebola with disappointing results. Initial trial findings appeared to suggest Remdisivir cut recovery times for severely ill patients hospitalised with Covid. But no trials reliably looked at whether Remdisivir could save more lives and lead to better patient outcomes than standard care.
In November 2020, the World Health Organisation (WHO) recommended against the use of Remdisivir on the basis of there not being enough evidence to suggest it improves outcomes for hospitalised patients. Given this is an expensive treatment, the cost-benefit didn’t weigh up for some health authorities. As such, the celebratory attention it first received quickly disappeared.
REGEN-COV/Ronapreve (Regeneron) – Monoclonal Antibody
REGEN-COV is a different treatment, not used in those with Covid19 but in those who have been exposed to it. It’s a post-exposure prophylaxis treatment, designed to help prevent someone from catching Covid and testing positive or being symptomatic.
This was authorised for use in the UK by the MHRA in August 2021, and was granted emergency use in the US. Developed by Regeneron Pharmaceuticals, Inc., the monoclonal antibody cocktail contains casirivimab and imdevimab, sold under the name REGEN-COV in the US and Ronapreve in the UK.
The FDA notes that REGEN-COV is for those at high risk of severe illness from COVID19 and who are either not fully vaccinated or are not anticipated to form an adequate immune response from vaccination, like immunosuppressed individuals. It’s for those exposed to someone infected with Covid, or at high risk of exposure due to the setting, such as an institutional setting like a nursing home.
Tocilizumab (Hoffmann–La Roche and Chugai) – Monoclonal Antibody
Tocilizumab (brand name Actemra, plus others) is an immunosuppressive drug typically used for the treatment of arthritis, including rheumatoid arthritis. It’s a humanised monoclonal antibody that targets the IL-6 (interleukin-6) receptor. It’s typically for those hospitalised with Covid19 to reduce the chance of death and aid recovery.
Findings have suggested that the “hyperactivation of the immune response, including release of pro-inflammatory cytokines such as interleukin-6 (IL-6)” could partly explain the pathophysiology behind severe illness after a COVID19 infection. Under this premise, the likes of dexamethasone, a corticosteroid, has been used. Tocilizumab takes it a step further by targeting the IL-6.
Earlier research was conflicted, but some of the variation in findings could be due to trial size, population and uncontrolled variables. The largest trial undertaken to date has been from the Randomised Evaluation of COVID-19 Therapy Collaborative Group, referred to as the RECOVERY trial. This looked at various treatments used on over 27,000 patients with COVID19 hospitalised in the UK. While more robust and more substantial than earlier studies, it still has its limitations.
This study discovered, among other things, that mortality affected 35% of patients who were allocated “usual care” and 31% of patients who were given Tocilizumab. Patients in the latter group were also found more likely to be discharged from hospital within 28 days.
UK : The Current PANORAMIC Study For Molnupiravir
In the UK, Molnupiravir is currently part of a national study, PANORAMIC. The University of Oxford in collaboration with GP practices started recruiting around December 2021 for 10,000 patients in the UK considered at high risk of serious illness if they caught Covid19. These patients would be offered Molnupiravir at home if they test positive on a SARS-CoV-2 PCR test.
This is just one treatment available for the purpose of research. It’s important to note that the highest risk patients in the UK outside of the study, including the likes of cancer patients, those with Down’s syndrome and the immunocompromised, should also be able to access Molnupiravir and Ronapreve from 16th December 2021 onwards, alongside other newly authorised treatments like Paxlovid. According to the government website, such treatments are to help protect the most vulnerable over the winter months in the hopes of reducing hospital admissions and thus also the pressure on the NHS.
Clinical trials have shown Molnupiravir capable of reducing the risk for hospitalisation or death for at-risk adults with “mild to moderate COVID-19 by 30%”. Ronapreve reduced this risk “by 70%”.

These two treatments offer patients a more convenient approach to protecting their health without requiring hospitalisation.
Individuals can sign up to the PANORAMIC study on the website, as well as at GP practices and NHS sites throughout the UK. It seems you can only sign up once you have symptoms and a Covid19 infection. It doesn’t appear that you can sign up in advance just in case you get infected.
Additional Treatments
Obviously this isn’t an exhaustive list. There are also the likes of the intramuscular injection treatment AZD7442 by AstraZeneca, an antibody cocktail the company claims can reduce the risk of hospitalisation or death when used within the first 5 days of infection by 50%. AstraZeneca also claims the drug could work as a prophylactic by preventing symptomatic Covid. Research results are still under review.
There’s also casirivimab with imdevimab, neutralising antibody IV infusions for mild to moderate Covid, in use in the US and the UK.
There are other drugs already in use for other conditions, as well as newly developed Covid-specific drugs. Some have been shown to be ineffective, others may still be tried given the lack of efficient, available treatments. This article just shows the main ones of interest and the ones hopefully accessible by patients in some countries. While developments in treatments and research continually evolve, it’s important to note that new findings and implications – for better or worse – are also being continually discovered.
Problems & Challenges With Current Coronavirus Treatments
Some of the treatments outlined here have shown promise and sparked a lot of interest, as well as gaining a lot of airtime in the press. So why can’t all patients access the “game changing” Covid19 treatments? Unfortunately there are going to be limitations to medications, as well as problems in the process of getting treatments to patients.
The current understanding of how COVID-19 develops and affects individuals, as well as research into current and new treatments, is constantly evolving. What may seem convincing and positive one day may come with scepticism or disappointing results the next, and vice versa.
Here’s a quick look at just some of the challenges and limitations with treatment of Covid19 at present:
- Stock and availability of many of these treatments are limited. For instance, Paxlovid is in demand given its convenience and seeming efficacy, but Pfizer just don’t have the stock or ability to produce more any faster than they are. In the US, despite a large order in the books, current supplies are much lower and have to stretch a long way, meaning individual areas will have very little. As an example, it seems Washington DC, with the highest rates of current cases in the US as of December 2021, will only have enough courses to give to 120 people.
- Treatment manufacture takes time. The US have ordered 10m courses of Paxlovid and 3m of Molnupiravir, and more orders are likely to follow. The situation is similar in the UK and elsewhere, with a wait period between ordering and receiving treatments because such drugs could take months to even manufacture.
- Cost, politics and practical implications mean poorer or less in-the-loop countries are going to be missing out and potentially unable to access these cutting edge treatments. On top of that, it requires the governing bodies to approve and then order such drugs, which is a long and complicated process.
- Merck’s Molnupiravir treatment appears less effective than originally hoped, reducing hospitalisation in high-risk patients by 30%, perhaps even less so against the Omicron variant.
- Paxlovid isn’t recommended for people with severe liver or kidney disease.
- Caution should also be taken when it comes to patients taking other medications. It’s believed that Paxlovid could affect how other medications work, including the likes of blood thinners, some antidepressants and statins.
- Paxlovid and Molnupiravir are to be taken as soon as possible at the onset of symptoms. This is a practical challenge with shortages of diagnostic tests, poor access to healthcare and GPs to prescribe treatment, delays with physically getting treatment to the patient and so on. The delays could thus reduce effectiveness and positive outcomes.
- Molnupiravir isn’t to be given during pregnancy in case the mutations to virus DNA harm the foetus or baby. Also, men hoping to start a family are advised to wait 90 days following treatment.
- Given potential side effects of Molnupiravir, the FDA has restricted its use to adults only in certain scenarios, such as where other treatments are inaccessible or not “clinically appropriate”.
- While severe cases of illness in the young are very low, there have been such instances of hospitalisation or death. There’s little in the way of Covid treatments for children; most outlined here are for adults only.
- Each medication is usually available in only one format, ie. A pill format for Paxlovid, with no same-brand different format replacement for those unable to take oral tablet medications. Roche is one alternative treatment that can be given by injection.
- Covid treatments are tools to be used to help reduce hospitalisations and deaths, they’re not a replacement for vaccinations. The legwork required by medical professionals, other staff and volunteers across vaccinations, diagnostic testing and Covid treatment will stretch already struggling healthcare services even further. This could lead to more delays and more obstacles for patients to get the help they need.
- It’s possible the virus could continue to evolve, mutate and evade vaccines as well as become more resistant to treatments.
★ ★ ★ ★ ★
Despite the challenges and limitations, current treatments are giving the world some hope and are helping in the fight to save lives.
Greater stocks should become available in 2022, further treatments are likely to be developed in time, and hopefully current and future mutations of Covid19 could be milder, much like it is hoped Omicron could be as it continues to rapidly spread.
Obviously, I’m not a scientist. The information presented here is only correct to the best of my knowledge and based on numerous online sources at the time of posting.
I hope nobody needs this information. But if you or someone you know is in the position of needing help, being aware of what is available is important. You need to know what you could ask about so that you can fight for your, or your loved one’s, health.
Caz ♥
Facebook || Twitter || Instagram


12 comments
Thank you for sharing this information and clearing things up. Vaccines and medicines and so many other things have been so confusing surrounding COVID. I understood that in the beginning but it’s been 2 years so you’d think they’d have things a little more figured out by now. This is a great article!
I didn’t know about all these things. Wow. There is so much misinformation it’s hard to know what to believe and what not to believe. Thanks for clearing up to many questions.
Have a fabulous day and weekend, Caz. ♥
Brilliant post as usual.
Very valuable information here, Caz! Thanx!
One of the problems here in the US is the extreme lack of this information in the mainstream media as our government seems obsessed with vaccinations and ‘punishing’ the unvaccinated as though they are criminals. While Anita and I are vaccinated, the overkill of our government on trying to force people to do so and mandating masks ignores any of this information you have provided. I found most of what you shared on “alternative media” such as Epoch News or podcasts.
❤️&????, c.a.
Caz, this is invaluable information – thank you.
I didn’t realise those were available and I imagine many others didn’t either. The problem is that some should be started within 5 days of symptoms. If people don’t know this information, they won’t get the treatment in time.
I hope that I don’t need to remind myself of this information for anyone I know, but I am so glad to know where to find it if I do!
Such a well put together informative post.
Take care,
Liz
Thank you for this. I’m shocked, but I guess I shouldn’t be, by the amount of people around me who either have it, or have been exposed to it. Just yesterday I found out about 4 who have been exposed, of course that meant that at least 5 people they have been in touch with had it. What the heck? Some of these people are elderly, others have lung issues, one is 14 months old! Luckily the later has very few symptoms, she’s running around everywhere. My neighbor is elderly and was exposed by her granddaughter, who is feeling very ill, not hospital ill, but really sick. She called her doctor to see what they should do, he said to wear a mask around anyone for 10 days and come in if they have symptoms!! WHAT?? She should be wearing a mask anyway!! (our county has a mask mandate, of course you can’t make people do it in their own homes) I thought she had gotten it through her head that she is not “free” just because she is vaccinated!
I have NO GUILT about cancelling the family Christmas now. This is insane!
I’m keeping my butt at home!
I wish I didn’t have to go to doctor appointments….can’t put it all off for years! But I’ll be masking up! With good quality masks! And Sanitizing!!
You stay safe my friend. You are always in my heart.
love to you
Wen
Great information! Effective treatments are key to getting back to normal.
Such valuable information! Thank you so much for sharing this interesting post, Caz.
Charlee: “We’ve never seen so many different treatments and medicines come out so fast!”
Chaplin: “I guess that just shows what humans can do when they’re in a corner and their backs are to the wall. Now if they could only figure out how to keep that from happening in the first place …”
I’m glad that these options for treating COVID are available, since we’re clearly never going to be rid of it at this point!
Thank you, Caz for such a comprehensive article about prevention and treatment of coronavirus. It is great to see the information all in one place. 🙂
Happy New Year, Caz!!!!!!! I hope this is an AMAZING year for You and Yours!!! Loving the new header! And wow….this is so wonderfully thorough. I seriously had no idea there were so many options out there at this point. It’s a wonderful service putting all of this in one place. Thank You!!! Sending huge hugs Your way! ????????????