For better and for worse, having an ostomy will change many facets of life. We never think it’ll happen to us but there are many reasons someone may find themselves requiring a stoma, be it temporary or permanent, and there are different types of stomas, too. The experience is unique to each person, and while some will say theirs has been a blessing and has given them their lives back, others struggle with acceptance, find it hard to manage and are plagued with problems. I’m going to share just 14 ways in which having a permanent stoma bag has changed my life.
[ This post is in honour of Stoma Awareness Day, October 7th 2023 ]
★ ★ ★
What Stoma Do I Have & Why?
I have an ileostomy, which is where the end of the small bowel is pulled through and out of the abdomen, and a bag is placed on the skin. In contrast, a colostomy is where the end of the large bowel is pulled through. I also had a colectomy, so the surgeons stole my large bowel. In the years since, I’ve had a couple of stoma reformations and bits chopped off my small bowel because of bowel twists. FYI, bowel twists hurt!
While I had problems with my large bowel and constipation suddenly and without explanation shortly before I turned 20, it wasn’t until I was age 26 and had my first surgery that things really went wrong. I’ve never spoken about this surgery and what it involved because at the end of the day I’m a hypocrite and simply too embarrassed. It’s hard enough writing about my stoma and other conditions, but maybe one day I’ll broach the subject. Anyway, this surgery was supposed to help, but I was naive and knew nothing about what it all was, what it involved, that it wasn’t really “safe” and simple as this surgeon had claimed. He said I had to have it, and like a fool I paid for it privately as suggested, when in fact I never should have had it done.
This surgery caused irreversible damage and I knew I was in a bad way, that I couldn’t keep going like that. Some time later I was told my only options were to wait to die, or to have a stoma bag. I opted for the latter, but it wasn’t an easy choice to make.
★ ★ ★
How A Stoma Bag Has Changed My Life
1. My Diet has Become Restricted
Ostomates are often recommended to have smaller but more regular meals and/or snacks because larger meals can be harder to digest. There are many typical recommendations on different foods to eat and those to avoid. Simultaneously, it’s also often suggested that you can eat as normal and enjoy whatever you want. Strange contradiction there, huh? But these one-size-fits-all approaches are total nonsense. Everyone is different. Some have no dietary changes with a stoma, some have significant ones.
I quickly learned a few things in the early days of having my stoma and it’s very much a process of trial and error over time. It’s not much fun when you encounter the errors though.
My stoma is prejudiced against various things, like most types of meat other than tender chicken and bacon. Oh how I’ve longed for a hot dog, a home made cottage pie with a huge side bowl of peas, a sizzling steak. Mmmm.
Fruits and vegetables are a bit hit-and-miss, so while many vegetables as well as bananas are a no-go, some fruits are oka, though I need to avoid skins on apples and grapes.
I can’t eat regular sized meals, which probably tended on the larger side, like I used to before all of this happened. Eating a regular sized meal is agonising and a few years later I learned a surgeon put numerous little metal screws in my back, which explained a few things. Once in a blue moon that extra agony may be worth it, but I tend to stick to the general discomfort most eating brings.
Then there’s the issue of cooking, which I basically don’t do anymore. Between chronic migraines, chronic pain and chronic fatigue, standing up and taking more time to make a meal in the evening seems hellish. Especially when you’re getting out pots and pans all for what can only be a small portion. Eating out can be trickier when your options are limited, too.
At least I can eat chips (or fries, to the Americans and Australians out there), drink Pepsi Max and devour plain chocolate like there’s no tomorrow, for which I am very grateful as these things can be a no-go for many ostomates.
2. No More ‘C’ Word
I developed sudden-onset constipation age 19, aka the ‘c’ word. I found it so embarrassing that I didn’t tell anyone other than my mum and the various doctors I saw over the years who continually brushed me off. What I didn’t know then was that my large bowel had died. I’m not sure if it happened at the beginning or part way through the journey but it meant nothing happened naturally and I had to rely on laxatives. Who knows how things could have gone if just one doctor had taken me seriously back then, had tried to help me instead of tell me it was all in my head or to drink more water.
I was so fed up with all the medical appointments and getting nowhere. I spent a fortunate on OTC tablets and it was difficult to manage the symptoms in between work, hobbies and socialising, especially in secrecy. But I did manage it, and I managed it for several years while I had boyfriends, entertained an active social life, enjoyed exercise and did work that challenged me.
With an ileostomy, I no longer need any such tablets. I don’t feel I ever really had time to acknowledge this because I had a lot of problems after my stoma and with other health problems thanks to that first surgery. While I can say I’m glad not to be on these tablets because nobody would want to rely on something like that, I can’t throw a party about it. I never should have ended up with a stoma. To play devil’s advocate, even if I’d only had the stoma and no original surgery, I would have fared a lot better. Less adhesions and less bowel twists, no autoimmune problems, no widespread inflammation, no nerve damage, no chronic pain. In reality, I’d go back to the ‘C’ word in a heartbeat if I could go back to being an otherwise healthy girl.
3. I’ve Lost Weight
After each surgery the recovery is slooooow. It’s hard to face food at first I was told to eat low residue, low fibre and extra small portions for 3 months after each op, but I’ve since been advised to do low residue for life given the risk and frequency of bowel twists, as anything that challenges my insides will up the chance of problems. With each A&E visit, I’ve usually had two days or more of nil-by-mouth. You go a week without eating and you lose a pound or two. It’s not a route I’d recommend for weight-loss.
Then it’s the same extra restricted diet, and not having the strength or energy to cook, so I rely a lot on snacks. The loss of weight from my large bowel having been pilfered by the surgeons, the loss of muscle mass that leaves me a bit of weakling. Furthermore, absorption can be problematic when you’ve no large bowel and a shortened small one.
Some people find they gain weight with a stoma, and these are often the people who’d previously been unable to eat well because of Crohn’s, Ulcerative Colitis or similar. The stoma gives them the chance to eat better again without the same pain. For others, they lose weight because of dietary issues, hospitalisations, mental health and appetite, or poor absorption.
Over the years for me it has been a bit of a yo-yo, putting weight back on, then losing it again from an A&E trip or surgery. I’ve lost weight compared to what I was pre-first surgery, but I’ve gained some back in the last two years and I’m okay with where I’m at, regardless of what the illogical BMI calculation judges me to be.

4. Bowel Twists Are The Norm
Each time you have surgery, you can get adhesions building up, which is essentially sticky scar tissue. It’s the adhesions that cause my bowel twists. They can be partial, as I can get most weeks and deal with at home just riding it out until it eases, or they can be severe and require A&E. I’ve also had a suspected ureter twist so these adhesions can cause problems with any organ or structure in the body. The problem is, having surgery to remove or reduce this scar tissue can in turn create more scar tissue. Go figure.
5. I’ve Lived In Fear Of A&E
I’ve been to A&E on a number of occasions now with the more severe bowel twists. I realise some people have had blessed and positive experiences, but unfortunately I seem to have had a lot of pretty bad experiences with hospitals, nurses and doctors. And that’s an understatement. I think it’s fair to say some of these experiences themselves have been traumatising. I’ve had to all but be dragged to the emergency room and I once told my mum I’d rather die in agony at home than go back.
I won’t go into specifics because I’ll be here all day but suffice it to say, the fear is real.
6. It Has Challenged Me To Be More Open
The early days age 19 were ‘normal’ aside from the constipation and yet it was a word I couldn’t voice. It was way too embarrassing. Even years later and I couldn’t say it, had to dance around it and hope someone got the general gist. When I had a stoma, I knew I could either shrivel up with humiliation, or I could open up about it a bit. Part of that is the ‘fake it til you make it’ approach and part of it is trying to see the funny side, to make a joke of the things that cause embarrassment.
In challenging myself, I first went to Wordpress and wrote the words on there. Then it got a little easier. It’s less easy telling people I know or people I used to know years ago, but you have to take baby steps. If someone doesn’t react well, that’s their problem.
Being more open can be hella empowering as much as it is scary, and it lifts a weight from your shoulders. Finally you can start to come out from the shadows, no longer having to try quite so hard to keep the secrets to yourself while living in shame and embarrassment.
7. I’ve Had To Get A Wardrobe Refresh
Despite often reading that you can “wear whatever you like” with a stoma, my stoma bag has necessitated a review of my clothing choices. A lot of my more professional work clothes have to go and there are still some I can’t bring myself to get rid of. Jeans are tricky as sometimes I want jeans a little lower because I hate things around my tummy now, but sometimes I need them a bit higher to cover the bag. Some tops are too clingy, some are too loose and make the bag more noticeable.
Weight changes mean what I put into a storage box two years ago now fit me, and the new clothes I just bought are now too small. It’s a nuisance. And that’s if you can even find a smaller size trouser or pair of pyjama bottoms that are also petite length and not designed for a 6ft woman.
The fibromyalgia and the feeling of discomfort in some clothes that are too rough or too tight have also changed what I wear around the house, but I’ll put up with some discomfort for going out because I can’t live in baggies or PJs all the time.
8. High Hernia Risk Requires Daily Caution
Once you have abdominal surgery, the abdominal wall can start to weaken. If you have a few ops in a similar area, that weakening will become more pronounced. I’ve had 7 ops on a similar area now and what with the stoma revisions too, I’ve been told I’m at high risk of hernia. In fact, the last surgeon I saw in A&E sounded very surprised I didn’t already have a hernia and I asked him politely to not jinx that by keeping saying it!
Hernia prevention is a case of being more cautious. Cautious how you cough so as to support your tummy, especially if you’ve got a chest infection and are coughing a lot. Cautious how you do day to day tasks like vacuuming or sitting up from lying down. Careful with exercises. Especially being careful with lifting things heavier than a full kettle.
For many people who get a hernia, it’s not a one-off repair because that weakness in the muscle and tissue remains and leaves them more vulnerable to recurrence. The best way is to do what you can to avoid a hernia in the first place. The problem is that sadly for some people, it still happens regardless and seems an unavoidable reality.

9. It Makes Me Self-Conscious
Having a stoma can make me self-conscious about the bag being noticeable under my clothes or noticeable in general, as well as the worries about leaks and needing to empty or change the bag. I’m also more self-conscious because I can’t always walk too well and it’s hard to stand up from sitting normally when out. I’m self-conscious because I try not to show pain or make it obvious that anything is wrong with me physically, and sometimes that’s really hard to mask no matter how practiced someone may be.
10. I Map Out Toilets Before Going Anywhere
For urinary issues like peeing a lot and having a stoma, knowing where the toilets are is a must. Lack of public toilets in many towns up and down the country and across the world. Thankfully supermarkets usually have toilets and if you’re in the centre of town, there’ll be the odd toilet block in a shopping centre or the single toilet in a cafe. The problem is you need to walk what feels like miles to find the damn toilet or you need to buy a drink for the pleasure of of not peeing yourself.
When it comes to stomas, emptying a drainable bag (what I use) is something you should be able to do in any regular toilet. The problem comes with needing to change your bag, so for people with closed stoma bags or for those with drainable pouches who experience a leak or another problem that requires a change, you tend to need a disabled toilet.
Cue the potential looks and comments from those who think you’re not disabled or you’re skipping the line of people waiting for the regular loos. Cue the embarrassment as you either try to ignore it, or try to stand up for yourself.
Even disabled toilets are often ill-equipped for ostomates. The likes of Colostomy UK are doing fantastic Stoma Aware campaigns to make stoma-friendly toilets the norm rather than the rarity. You need somewhere to put your kit next to the toilet at the very least, and a grimy floor where it’s hard to reach is not the answer.

11. Travel Is A Practicalities Minefield
Any chronic condition or disability is likely to require extra thought and planning when travelling, whether it’s a day out or a holiday abroad. With a stoma bag on a day trip, it’s good to figure out where the toilets are, take your radar disabled toilet key and make sure you have supplies in case of an emergency, which may include a spare top or change of trousers if you’re more prone to leaks. If you’re going away for a few days or a few weeks, you’ll need a lot more supplies to keep you going.
Holidaying abroad is a little more complex. From travel insurance, getting a stoma nurse to sign off on extra supplies to be prescribed and figuring out what the healthcare system is where you’re going, to sorting decent travel insurance with pre-existing conditions, arranging additional baggage with your travel provider and pre-requesting any additional support required with the airline before the trip.
The end result? A LOT of luggage, all thanks to medical supplies. And I wouldn’t need half as much as some people do.
I went to Spain two years after the surgery that tanked my health and it was very difficult physically, but it felt like a now-or-never situation, one that I didn’t think I’d be alive to see. My mum dearly wanted to go abroad for a holiday as she’d not really had a proper trip like that before and seeing her enjoy it was wonderful. Thinking about it now, I’m not sure I could face a holiday again, not just because of the cost and the stress of it but simply not feeling well enough to go through it all because of other health issues. But it is doable for many with a stoma, it just takes some working out.
12. Sometimes I Can’t Face It
I’ve had my stoma for a good couple of years now. You’d think I’d be used to it, accepting of it and totally okay with dealing with it. Wrong. Sometimes, I can’t face changing my bag routinely, and having experience with changes that do not go swimmingly well is rather off-putting too. Sometimes, I don’t want to have to look at and sort my supplies.
Sometimes feeling like I can’t deal with it at all and don’t want to acknowledge the situation can mean I simply can’t face it for a while, and it’s a regular occurrence. Having a stoma for more than a year or two doesn’t necessarily mean you’re okay with it, at least not all of the time, and it certainly doesn’t mean you have to be happy about it. You do whatever you have to do to manage, and you can’t let anyone else tell you how you ‘should‘ feel.
13. I Feel Traumatised
The first surgery I had, which was pretty diabolical, deeply affected me even though I’ve tried not to let it. You can’t help it. Your experiences can change you and they can stay with you when you don’t want them to. After that, I’ve gone through a lot of complaints procedures, dealings with the GMC, a legal case. It all added up. Then comes all the other doctor, surgeon and specialist appointments, so many of which were traumatising in their own right. A&E experiences that bordered on the outrageous, things that were said and done that I can’t forget and that have caused such a mix of emotions that I don’t ever want to go back. Not that we get much of a choice when we need emergency care.
During the legal case, a psychologist gave me her diagnosis: PTSD and severe depression. I found it strange to read that report and see those things said about me. I think when I stay busy – to whatever degree I can when I lose a lot of time being unwell – it helps me push the important things to one side. I can be a little ignorant of it all, I can pretend I’m okay more easily. I can laugh things off, or I can get so angry and use that anger it to do something about the situation. But underneath all of that is what I don’t really want to admit to. That I’ve been terrified, that I’ve lost every last shred of self-respect, that I feel humiliated, that I feel burning rage when I hear of other injustices and patients suffering, that I can’t rest or shut off properly, that I’m jumpy, that sometimes I feel nothing and other times I feel everything.
14. I Rely On Humour
When I was 16, I had my first ‘proper’ boyfriend. He was very much a fun-loving, easy-going guy and it was a breath of fresh air for someone like me who was so shy. He made me realise, and be able to put into practice, that sometimes you need to make light of things more often. By laughing it off, by actually talking about something you don’t want to, by acknowledging an issue that’s embarrassing, you’re taking the impetus and fear and taboo straight out of it.
With a stoma, and with other health issues, I try my best to laugh it off and make jokes where possible. I started doing that for my parents so they thought I was okay and to make them feel more comfortable. But then I found it helped me, too. I don’t think I could talk about it at all if I didn’t joke here and there.
A stoma is serious issue but if you’re feeling closed down and afraid, facing it head on and taking it in jest briefly can really help. If a little humour is helpful, roll with it. After all, ostomates are pretty special because not everyone gets to see and speak to their insides every day!

If you have a stoma, is there anything you would add about how a bag has changed your life?
Facebook || Twitter || Instagram


26 comments
Thank you for your uncommon openness, honesty, courage, and generosity of spirit. Your inspiring words are spreading hope and strength farther and wider than you can ever know. 🌻
You’re most beautiful. I wish I could give you a hug. I think you’ve handled the cards you were dealt very well. Good for you.
Have a fabulous day and weekend. ♥
I hope the next few years are much better for you than the last few
Thank you for this candid look into your life, Caz. xo Your courage, I’m sure, has helped so many people. One of my best friends has an ileostomy and a close family member has a colostomy. Because I was an RN, I’m the one who took care of this family member (gladly).
I can’t tell you how much this article means to me. And, girl, you are hot in that bikini! 🤍🌻🌺
Your ability to describe all the complexities your health has foisted upon you seems to me remarkable. I’m sure this candid piece is helping others with stomas and is raising awareness among so many readers. I just hope the writing gives you some measure of comfort. You deserve the very best, dear Caz.
XXXX annie
Thank you for your candidness. As others have stated here, you are beautiful and I would add inside and out. Your generosity of spirit is a gift to others of us. I will be having open heart surgery later this month. It scares the hell out of me. Stay strong. 🖤
Can I simply say that you are brilliant, Caz. You encourage me no end with your tenacity and humour. And with your ability to explain the detail of your health challenges and be so thoughtful of others and informative with it. I have no doubt you help countless people without realising. Love & gentle hugs, Penny xxx
I can relate to so much of this post! My husband had surgery on his intestine and had to have a stoma for three months. It was taken off two years ago and he still struggles with bloating and constipation issues. Thank you for spreading the word that these kinds of procedures have long-lasting effects!
Oh Caz!!! I so agree with that young man who advised “to make light of things more often. By laughing it off, by actually talking about something you don’t want to, by acknowledging an issue that’s embarrassing, you’re taking the impetus and fear and taboo straight out of it.”
Anything that’s kept secret or ‘hidden’ has enormous power over us; power to cause us harm, that is. What a wise young man he was.
I do appreciate your embarrassment and desire to keep much of your story to yourself. I appreciate the anger you must feel at the complete incompetence of some doctors. Oh sure, there are some good ones, no doubt. But, there are also the nincompoops (as in all walks of life) who should not be practising. Bugger, if only acceptance came easily. It does not. But, what can we do, but accept and move on…
Write on, Caz. It will not only do you good; it will be good for others too.
Wishing you all my best.
xoxoxo
Caz, you are one special person. I’m sure this post will help many people. You are a beautiful girl and so smart. The world needs more just like you.
Caz, Thank you for sharing this information. It is very generous of you to promote understanding of your health issues. You never know how many people have been helped by reading about your experience. <3 <3 <3
Lulu: “We know how hard this must be for you but we think it’s great that you’re sharing this information with the world.”
Java Bean: “Sí! The more people know, the more they will understand about what people may be going through, that they have no idea about. At least some of them, anyway!”
Caz, such an open and honest post. The angering part is that life might have been different if it hadn’t been for that first surgeon. That wasn’t your fault and you’re certainly not a hypocrite for not sharing more about it. You don’t have to. Only ever share what you’re comfortable with.
You go through so much but through it all, you help other people by sharing posts like this. Your voice will help others to feel less alone. It will also help people to understand that life with a stoma isn’t the same for everyone.
Brilliant post, Caz. Keep being you.
Liz x
I got a tiny taste of what this sort of thing might be like during my first few weeks home after The Event, when I was still catheterized and had a little bag (AKA “The Hip Flask”) strapped to my thigh. Of course I was pretty much housebound (except for doctor visits) so I didn’t have to cope with being out in the world while it was going on, as you have done and continue to do in your most amazing fashion.
Caz,
Thank you for your courage. Sharing your experience helped me to better understand what your life is like. It is a small window but still a window that will help me to be more compassionate toward what others may be going through on a day-by-day basis.
Please send me an email if you ever want to meet on Zoom to try writing together. Poetry has gotten me through my darkest days. It is not about writing great poems more about being heard. This is a gift I would like to offer you. No worries if you aren’t interested.
Wishing you all good things,
Ali
Thank you so much Caz for sharing your experience about having a stoma bag and being so honest and open about it. I am with you when you say you just have to cope with it, but this doesn’t mean you have to be ok or happy about it. This is a great post to raise awarness about this important topic.
Oh Caz, what an insightful and honest blog post. Thank you so much for sharing your stoma journey & just some of your dreadful medical experiences. I’ve learnt so much from this post & you being so open about it I’m sure will help other people on this rocky road of chronic illness & pain, thank you x
And the frowns you get when using the disabled toilet! Stupid, ignorant people.
My dentist complimented me on my figure recently, why can I look like this, she said.
I said, you have your colon removed and voilà. Her facial expression, priceless.
😂😂😂 I wish I could have seen that expression! Good on you, B. Sometimes we have to say something, and sometimes that makes us feel a tad better (I think so anyway, otherwise you’re swallowing everything down). I got something like “look at your little tummy, such a good figure” from a nurse once and I said “getting sick is the fastest way to lose weight, and if you want a flatter tummy, just get your bowel removed.”
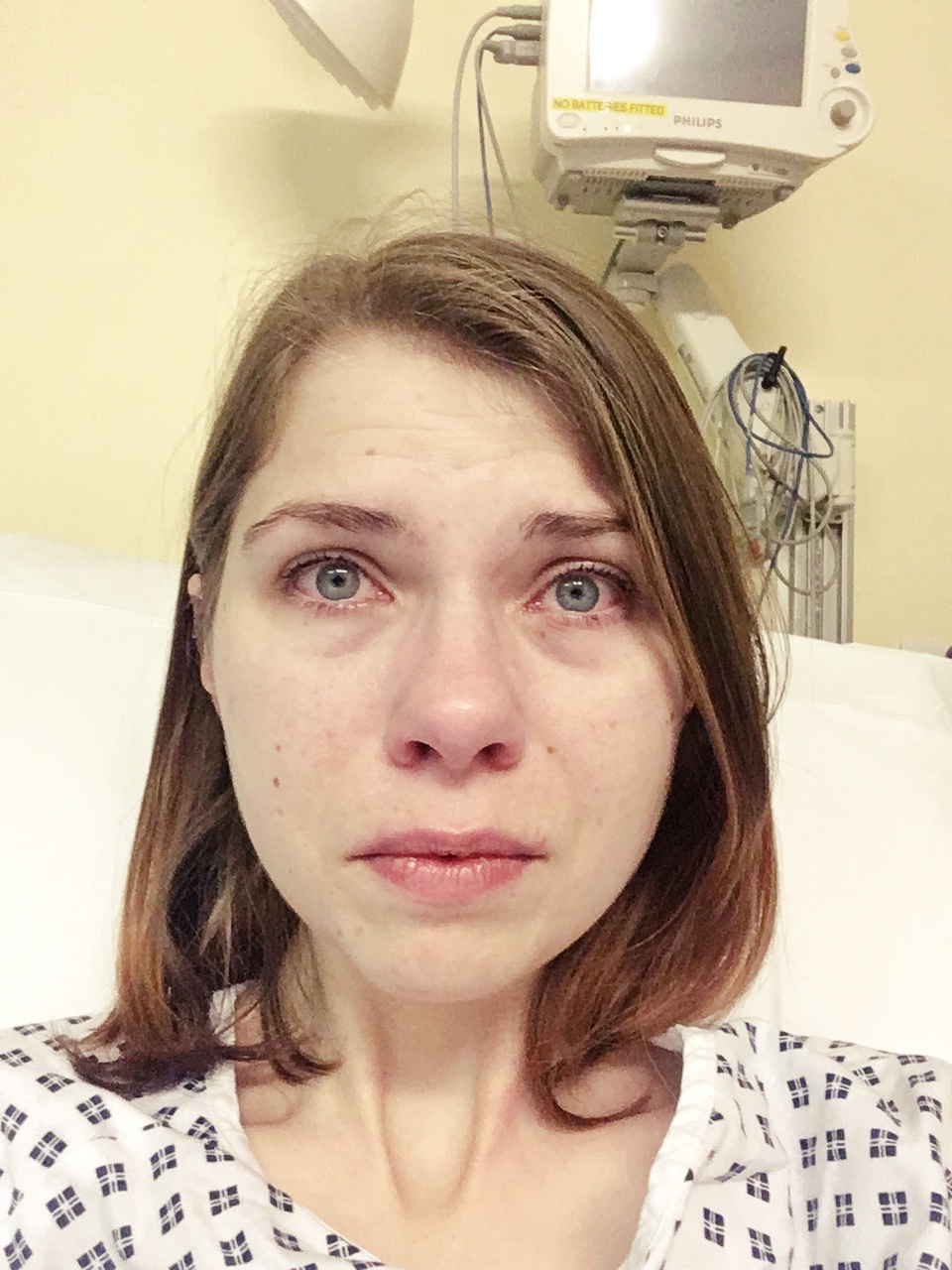
Hi Caz, Thank you for writing about this so honestly. I have learned so much about the things that you have to go through and live with and it is heartbreaking to see you look so upset in your picture from a couple of years ago 🙁 I am sorry that it was treated so awfully.
Your writing will help so many other people to not only understand what it is like living with a stoma, but also make others feel understood and not so alone. Although we do not have the same illnesses, they both come with relatable challenges, such as difficulties with travel planning and, of course, sometimes not being able to face our illnesses. Sending love xx
Thank you Caz for being vulnerable in so many ways, and I can only imagine how hard this one was to write. I appreciate your honesty, frustrations, and wishes for the future, present, and past. You are helping more of us understand what having a stoma bag means on a daily basis. By the way, I totally relate to not being taken seriously by doctors. As soon as many of them find out I have anxiety, they write off my physical concerns about my body. Thankfully a few have taken me seriously and led to diagnoses.
That angers me so damn much, Christy. I’m sorry you know what it’s like. It is sickening the way mental health is so often used like a broom to sweep any thought of physical health problems under the rug. If you don’t have anxiety, they’ll say your physical problems are due to anxiety. If you have anxiety already diagnosed, they’ll stop listening because they’ve already decided that must explain it all. Thank goodness for those odd doctors in between who actually listen, care and think things through beyond textbook definitions, prejudices and ignorance; I’m glad you’ve seen some of those doctors so you could get some answers and help. xx
Your post on “14 Ways a Stoma Bag Changed My Life” is a powerful and insightful reflection on the challenges and transformation that can come with health-related changes. Your openness about your experiences is not only brave but also educational. It provides a window into the world of those with stoma bags and offers support and understanding to others facing similar situations. Thanks for sharing your story and offering hope and inspiration to those who may need it. 💪❤️🌟
You are amazing. I bet this post alone has helped – and will help – so many people. Thank you for your bravery in sharing your experiences with us.
Caz, you’re an amazing friend. Thank you. It’s been over a month since you published this. I’ve read it three times. What a wonderfully deep insight into your world. There was very little I didn’t know except for the parts about the figure, but you made it more of a person than an information video. Please know that I care and understand your feelings.
[…] Caz is also an amazing advocate for hidden illnesses and regularly posts about the – unfortunately taboo – reality of living with a stoma. […]