BMI has long been used as the gold standard for categorising someone’s weight. Research uses it, gyms use it, healthcare services use it. But there are some pretty significant flaws in the use of BMI calculations that raise the question of whether it’s really suitable. Is it time for BMI to be scrapped in favour of an alternative method?
What Is BMI?
BMI stands for Body Mass Index. It’s a measurement that uses a person’s height and weight to calculate a numerical result, which is then categorised. In a nutshell, the result is labelled as being healthy or unhealthy due to being under or over weight. A “healthy” BMI result is between 18.5 and 24.9. The categories are based on averages and ideals because there’s no scientifically objective value for a weight that equals good health.
BMI is often used by medical professionals to quickly assess whether someone is a healthy weight or not for their age and height. While some doctors may take into account limited variables that affect weight, the basic result is often taken at face value.
How Do You Measure Your Body Mass Index?
To calculate BMI, divide the weight in kilograms by the height in metres squared. This needn’t be done by hand as there are online BMI calculators to quickly work this out for you and show where the result falls on the weight continuum. Some home bathroom scales or scales at chemists and gyms can also calculate BMI.
Most calculators will want the following information: Height, weight, age, sex, ethnic group, and potentially activity level.
You can find your BMI using the NHS BMI Calculator here.
There are 4 basic ranges that show if the result is underweight, healthy, overweight or obese :
- Below 18.5 : Underweight Range
- Between 18.5 – 24.9 : Healthy Range
- Between 25 – 29.9 : Overweight Range
- 30 and over : Obese Range

What Are The Implications Of Its Use?
BMI is used as a tool and means of categorising, judging, inferring and making decisions on behalf of individuals and patients. For patients, BMI is what is used to tell you “if you’re a healthy weight”. If you’re classed as not being at a healthy weight, BMI is used as a starting point for further advice and action.
BMI can feature in research, and that research can go on to dictate clinical practice. It can be featured in giving risk estimates to individuals, including school children, regarding the dangers of obesity if their BMI puts them in the overweight category. It can be a factor in decisions about whether someone is eligible for healthcare services or treatments.
It is also used as a method for assessing the general population via surveys and medical records to see the proportion of those who are overweight as part of the “fight against obesity”.
You’ll notice that the focus is often on obesity and the underweight category is often sidelined.

There’s an assumption made that a “healthy” or “normal” weight and BMI equals overall good health generally. That’s not always the case. Overall health is a complex picture that includes things we cannot control like our genetics. It also includes personal choices and lifestyles, which can be independent of weight.
For instance, one individual may live a healthy lifestyle, have less health complaints, and be physically very fit but have a higher BMI and is thus classed as being less healthy. This is in comparison to someone who is slimmer and within a “healthy” BMI range but who is chronically ill and with various health complaints, or who has a less healthy diet and lifestyle that actually puts them at far greater risk of further health problems. The outcome is that the first person may be cautioned about their weight without due cause and the second person can have potential concerns overlooked on the basis that they look “fine” and have an average BMI.
So if so many things are heavily reliant on BMI, and this method of calculation is crucial to research underpinning certain elements of healthcare systems, we need to be confident in the accuracy of it. If BMI turns out to be flawed and inaccurate, everything that follows on from that – everything that uses BMI in some way – will likewise be flawed.
The Flaws & Limitations Of BMI : What It Doesn’t Tell You
BMI calculations are very basic. It allows for a speedy quantitative result that conveniently fits into a graph or a tick box, but life isn’t that simple and neither is “health”.
Here’s a look at just a few limitations and complications that suggest BMI can provide an incomplete or inaccurate picture :
- Waist size is often thought to be an indicator of health, with more fat being carried around the stomach related to a higher risk of conditions like type 2 diabetes, stroke and heart disease. A person can have a healthy BMI that suggests they’re a normal, healthy weight, but their hip to stomach ratio or waist measurement can suggest otherwise.
- BMI cannot tell the difference between excess muscle, fat or bone.
- Your BMI can tell you if you’re carrying too much weight, but it cannot tell if you’re carrying too much fat.
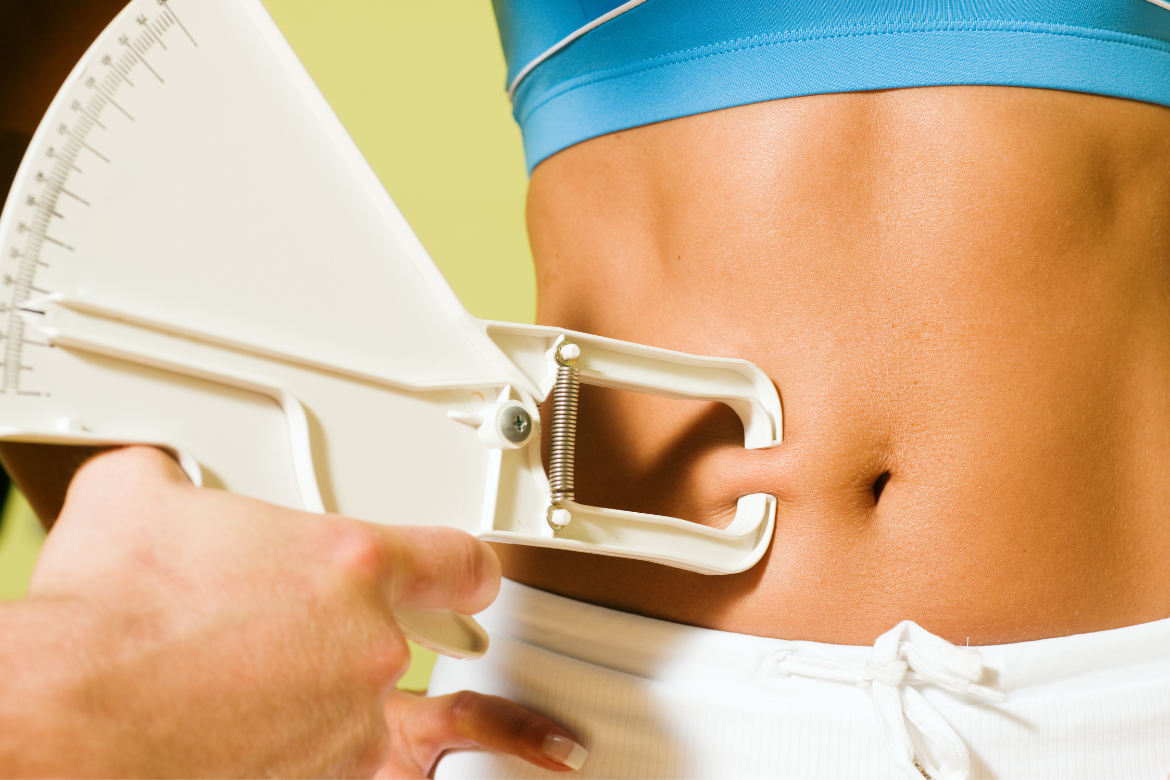
- The adult BMI does not take into account muscle mass. This means that very muscular adults and athletes may be classed “overweight” or “obese” even though their body fat is low. Meanwhile, adults who lose muscle as they get older or through chronic illness may fall into the “healthy weight” range even though they may be carrying excess fat. Someone could also be classed as being underweight when lack of muscle mass isn’t taken into consideration.
- Alongside muscle mass is bone density as a personal variable. The higher the density the heavier the skeleton will be. Conversely, those with osteoporosis will have less bone weight than someone with average density for their age.
- Another individual variable would be missing body parts. Having an appendage amputated or the large bowel removed, for instance, would reduce a person’s weight.
- Pregnancy will also affect a woman’s BMI result. Your BMI will go up as your weight increases. You should use your pre-pregnancy weight when calculating your BMI.
- Weight is not a measure of health in and of itself. A heavier individual could be far healthier because of their diet and lifestyle than a lighter individual, but based solely on BMI they’re classed as having a problem and of being at higher risk of conditions like diabetes.
BMI is a relatively straightforward and expedient way of assessing someone’s weight. The fact that it doesn’t give a full or reliable picture of the health of someone’s weight is what puts a question mark over the consistent reliance on BMI.
Calls For BMI To Be Scrapped
MPs have recently criticised the use of BMI in determining the healthiness of someone’s weight. They’ve called for the measurement index to be scrapped, and furthermore called the government’s obesity tactics “dangerous”.
There’s a concern that the UK is turning into a “nanny state” and I personally think that many strategies employed, such as shrinking chocolate bars and ready meal sizes or adding sugar taxes, make the situation worse. The more miserable people become, the greater the likelihood of reaching for junk food or overeating. The more focus there is on fat, calories and health foods, the greater the likelihood of eating disorders, obsessions and anorexia. All too often, strategies are more about political statements, box ticking exercises and money rather than anything to do with public health or common sense.

The NHS significantly integrates BMI for children and adults within healthcare. It brands adults as needing to lose weight or put on weight on the basis of their weight and this BMI calculation alone. The suggestion is that a person isn’t healthy and the weight isn’t healthy because it doesn’t fall within a certain range. Schools have been increasingly called out for deeming some children as being “overweight”, while they appear to be a normal size and are otherwise healthy.
Parents are understandably outraged and there is real concern that body dysmorphia, calorie counting, self-consciousness about weight and eating disorders will all proliferate in any age group as a result of BMI reliance and the focus on weight and obesity.
One suggested alternative to the body mass index is the waist to hip ratio to determine fat distribution. The waist-to-hip ratio is calculated by dividing the circumference of your waist by the circumference of your hips. A high risk level of visceral fat, which can increase the risk of type 2 diabetes, falls within a different range for men and women : For women it’s a ratio of 0.85 or more, and for men it’s a ratio of 0.9 or more. But even this doesn’t tell you the whole story of health and weight. Nor does it put the focus on the underlying issues around being under or overweight, which is not just about access to fast food and chocolate. Until strategies tackle those underlying issues and dispel stigma around eating disorders and “fat”, the situation will remain unhealthy and ill-advised.
★ ★ ★
It seems it may be time to ditch the convenience of limited and potentially harmful quantitative data for a more equitable and realistic alternative. Weight and healthiness do not necessarily go hand in hand and the issues are far from black and white. It’s all very well to put a tick in a box or berate those who don’t fit within the ideal category, but if it’s not accurate, not useful and not fair, then perhaps it’s time for a change.

Do you think BMI is an unfair or unhelpful way to categorise weight & health?
Caz ♥
Facebook || Twitter || Instagram


47 comments
Great topic!!! You know I never thought about until reading your article. But I think it should be scrapped also. Why should we put so much value on BMI and not on educated everyone on better eating habits. Restaurants have bigger portion size than ever before.
This would be a great topic for a podcast, because there is so much to say here.
I’m glad the post made you think about it – I just wish the medical professionals & government bodies would because they’d also realise it’s time for a change. You’re right, education earlier on would be best, and I think there should be a deeper emphasis on emotions behind eating. That’s where the crux of a lot of problems, from obesity to anorexia, reside. I’d love to rant about this stuff all day but I have a face for radio and a voice for silent TV, so nobody would want me on a podcast 😂 Thanks for the comment lovely – I hope you’re having a good week so far! xx
No!!!!! Don’t say that about yourself. You belong wherever you are comfortable being. I agree it’s time for a change!!!!
Yes. It should be scrapped. Telling someone who is overweight could cause psychological harm. We don’t all fit neatly into little boxes and other factors, like you said, should be considered.
You’re right, we don’t fit into neat little boxes and other factors can’t just be ignored. The psychological damage should also be considered, especially when we’re talking young kids and teenagers. It’s dangerous and it’s not helpful if it’s not accurate. xx
Yes. Thanks for the helpful write-up!
A lot of people seem to agree that it should be scrapped – thanks for adding your opinion!
I don’t know what to think about this, than I know it’s been a debate for some time this method. The bmi causing problems. Especially with children.
Although medical settings are known to use it, it has only ever come into conversation with them, to me, I think twice. Somewhere around my late teens to early 20’s.
I remember the second time it was used, I was 9 and a half stone and it was suggested I was underweight.
I argued it because I said the bmi scale must have changed because when I used it at school in a lesson, I wasn’t then for the same weight and height.
Do you mind my asking what your height is? I was 9st9lbs at one point in my teens at 5’3″ and technically classed as overweight, yet I look back at photos as I never looked overweight, just healthy. I’d give anything to go back to that and still be healthy. It’s strange they classed you as normal weight at one point and underweight at another, despite being the same weight and height both times! Yeah, doesn’t make much sense!
This is an interesting article and something I had never really thought of before. I think medical people use BMI because it makes it easy to put someone in a box, but I agree with you that it isn’t an accurate measure of health.
I have personal experience with how medical staff make false assumptions based on BMI. My BMI would make me overweight, yet I’m active and in overall good health. I remember a few years ago going to a biometric screening clinic at work. The first thing they do is weigh and measure you. The nurse noted that my BMI was around 26, I think. Then, when she took my blood pressure, she kept fiddling with the machine and shaking her head. I asked if there was a problem and she responded “This can’t be right. It’s telling me you have low blood pressure.” I told her that my blood pressure has always been low. She obviously assumed that someone who was considered overweight couldn’t possibly have low blood pressure.
You’re right, it’s a quick and easy box-ticking exercise that fits people into neat categories. That can be helpful to a degree, but the limitations don’t often seem to be acknowledged, nor do the potential dangers. I’m sorry you’ve had BMI-based assumptions made, too. Clearly weight is not a useful indicator of overall health, activity and wellness, and as such assumptions should not be based on it. I’m glad you gave that nurse a surprise with your low BP! 😉
The waist-to-hip ratio to measure fat distribution may not be any better than using BMI to measure weight. Healthy women who have had multiple children with stretched abdominal muscles, or individuals endowed with broad hips may have skewed results. Also, individuals who were previously overweight and have excess skin, may not be measured fairly. Thanks for the interesting duel between the two methods to monitor weight.
Such a good point, Nancy. Many medics are saying the ratio is more appropriate as excess fat around the waste is often linked to increased risk of health problems like coronary disease. It’s another flawed approach as while it may be more effective in one way, it again fails to take into account other variables, like you say when it comes to individuals with naturally more broad hips or women with stretched abdominal muscles, those who’ve got excess skin from weight loss, or those with hernias, etc. I wanted to give a more clinical view of the issue in the post but I personally don’t think any of these old or new methods are up to scratch for suggesting someone is a “healthy weight” or “healthy” full stop. Parts of each may be helpful in some ways, but they’re riddled with holes and they need to be used with caution. Thanks for such a thoughtful comment, Nancy! xx
Lots of ‘food for thought’ here, Caz. I agree there are a lot of loopholes in the BMI system; so much so that to suggest someone falling within the ‘suggested range of health scale’ is rather fragile at best.
Here’s hoping you are doin’ OK… Sending Lots of Love
xoxoxo
Very fragile, indeed. I get what the medics and governments want when it comes to the benefits of BMI as an easily quantifiable measure that ticks boxes, but it’s not adequate and it can be dangerous. It peeves me that it’s often taken at face value without accounting for the individual variables. Thanks for the comment, Carolyn – I hope you’re having a relaxing weekend lovely! 💜
BMI was created in the 1830s for the Belgian government to use as a tool to measure obesity and health. It was created by a mathematician from numbers. In our supposedly advanced medical system it is still used to determine health.
I wasn’t sure of the origins other than the 1800s (though still earlier than I’d imagined) so this is brilliant, thank you for sharing! Your brain is a safe harbour for interesting facts to reside. You’d be good on a TV quiz show, George 😉 Having something easily quantifiable that fits in a spreadsheet or pie chart is very appealing for governments and healthcare services alike, but it’s not helpful when it’s riddled with holes and hidden dangers. I’m personally don’t think any old or new methods of measuring the healthiness of weight or health full stop is adequate; they may all have their benefits, but none is wholly accurate because they can’t account for all individual variables to tell the full story.
Indeed. Another factor is simply if the person feels good. 😎
Caz, this is a fantastic article. BMI is an absolutely crap way of determining someone’s health. We are all built differently and BMI cannot see that. There are so many more factors to be taken into account.
Oh, yes, we’ve become such a nanny state with the sugar tax and portion sizes reduced. And I think restaurants are going to have to start displaying calorie counts on menus. I worry that this is going to bring about a lot more people with eating disorders. It’s great to have advice about healthier choices but are people going to sit in a restaurant worrying about how many calories they’re allowed? Surely, that takes away any enjoyment of eating in a restaurant?
It is crap, isn’t it? I understand the appeal of an easy tick box exercise and to gather quantifiable data for the government or research, but using it as though it’s accurate and basing decisions on it is pretty stupid. Given how limited it is, I’m surprised it’s still so heavily relied upon and those limitations are rarely, if ever, considered. You’re absolutely spot on about the “nanny state” and the actions taken supposedly in the name of our health and the so-called “obesity crisis”. It’s all BS. It’s politics and money, and the calories on menus is a bit bizarre. If you want to know the calories, a lot of places offer that info on the website or you can guestimate it. No need to ruin the meal by calorie obsession, which doesn’t just ruin a meal, it’ll ruin lives. I’m so sick of it and I’m pretty sure that if multipack chocolate bars get any smaller there’ll be nothing left, we’ll be buying chocolate-scented wrappers to sniff. They don’t think of the crux of the issues and the more miserable we all are, the more eating disorders, anorexia, overeating and obesity will worsen. Eugh. Brilliant comment, Liz, thank you! xx
Since I live in the States, I hadn’t realized how much importance the NHS put on a person’s BMI. Since it really isn’t an accurate indication of a person’s overall health, I think it is past time to scrap it!
I think even if you lived in the UK, you might not realise unless you’re a weight that could be “unhealthy”, at which point BMI can be shoved down your throat as though it’s the holy grail of accuracy. Totally agree with you, it’s past time to ditch it (and preferably not to start relying on an equally limited & skewed method to class someone as healthy or not just to tick some boxes!) xx
I think BMI as a general guide had its pros: very high or very low and there’s likely a problem healthwise. However, slightly low or just above “normal” could be for any number of reasons and should be considered in the context of overall health. For children, it’s not the school itself but the school nurse representing the local authority who report on BMI. I remember large boy’s friends’ parents totally freaking out that their 4 and 5 yr old children had been categorised as overweight – awesome way to give young children a complex about their eating and appearance. On the flipside, large boy was in the bottom 10% but not flagged as underweight because the thresholds aren’t/weren’t applied evenly at both ends of the scale. So I realised where he was and myself freaked out that he was too slim. Needless to say, that cohort of 30 children remain equally healthy whether they were over or underweight 7 years ago.
It’s a good way to quickly collate quantifiable data for the government, health bodies and research purposes, and you’re right about how it can be useful health-wise as a general indicator. Then again, I think it’s more obvious if someone appears more underweight or overweight, so I’m not sure BMI is needed in that way, but you make a good point about those falling in the “slightly” above or below ranges. I hadn’t realised how they do it with schools but I’ve read about kids getting classed as overweight when it’s clearly not true or helpful in the slightest. I’m sorry for large boy’s friend’s parents getting such a shock, and you too thinking yours was a little underweight. It doesn’t always equate to healthiness, and the assumption is does seems pretty dangerous. Thanks for sharing your thoughts in such a brilliant comment! xx
Hi, Caz.
Your always thoughtful blogs keep us thinking! The best rating for health is simply discussions with a good family practice physician or general practitioner. No one gets guarantees of tomorrow, even if appearing in perfect health!
James Fixx, who started the Running craze in the USA, died suddenly of a heart attack at only 52 years old doing what he loved best – jogging!
Buddy Holly died in a small plane crash at the beginning of the peak of his career at only 22 years old.
Your own Princess Di passed away at 36 in a tragic auto accident.
Brittanie Cecil was a well rounded 13-year-old hockey fan in Columbus, Ohio, who died when struck by a hockey puck!
And the list could go on, of course, but you get the idea.
This is why it is so important for everyone as soon as possible to know where they will be after they die.
You and your family are in my daily prayers.
yours and His,
c.a.
It’s always mind boggling when seemingly very health, fit and active people die, often of heart problems. You’re absolutely right. And if it’s not that it could be a freak accident or just about anything else. You never do know. That’s so sad about the 13 year old Brittanie who was hit by a hockey puck 🙁
This is another great article Caz! Before I comment on BMI, I need to caveat my comments with the disclaimer that I live in the US, and although our healthcare providers do use BMI, there doesn’t seem to be as much an emphasis as you’re describing with the NHS.
My feelings about BMI are a little mixed. As a Personal Trainer, I often figured BMI for people, but I would always explain that it was only one data point in a lot of different factors when it came to their fitness. That was NEVER the only type of screening we did to determine their fitness level.
Like any tool, BMI can be a useful starting point. As Smelly Socks and Garden Peas said above, “BMI as a general guide had its pros: very high or very low and there’s likely a problem healthwise.” BUT this initial-use tool needs to be combined with other tools – like common sense, other measures of health, etc. – in order to really be useful. When we use just one data point to reach conclusions, those conclusions are often flawed, and BMI should definitely not be the only data point used when it comes to something as important as our health.
Thanks for giving us something to think about, and bringing attention to the fact that BMI doesn’t always tell the whole story.
I knew you’d be well schooled in this and would take that into account dealing with clients. I wish medical professionals as well as governments and healthcare bodies would also realise it’s only one tool and one part of the picture. It’s excellent as a quick, easy and visible result to give a general idea, but it’s by no means complete or accurate to state how healthy someone is.
Thanks for your comment, brilliant as always, Terri! xx
I think BMI can be useful to an extent. It’s good to have a rough ballpark estimate about where you’re at – for that reason I think BMI is still useful. But is it accurate? No. And for that reason I would agree that BMI isn’t the best method to get an accurate measure of health. BMI would suggest I’m healthy weight but my abdominal fat % would suggest that I am overweight.
Totally agree with you. It’s useful for that ballpark, rough idea but it’s not the full story and it’s not accurate. I don’t think the current reliance on it or the way it’s used, like by schools to tell young healthy-looking kids that they’re overweight (!), is really suitable anymore. We need a new approach, or at least one that recognises BMI isn’t all it’s made out to be. Thanks for your comment – I hope the week is going well for you so far! 🌸
Another thoughtful and valuable post, Caz. I haven’t seen much written on the topic, and you make a compelling case for skepticism, certainly.
Note: I was able to access this post via Reader. Hooray!!
Anniexxxx
Hurrah, so glad you’re now able to view the blog okay on the WP Reader! Technology, eh? 😉 Thanks for the comment and I’m glad my rambles on BMI made some kind of sense. It does worry me that it’s being relied upon and used in ways that aren’t really appropriate when you consider that it’s not the whole story and it’s not even accurate! I hope you’re keeping well and having a good week so far 🌻 xx
I think it should be kept as part of a range of tools to indicate health BUT should be adjusted for certain factors, eg ethnicity.
As an example: Weight that looks completely normal on a Caucasian person often looks obese on an Asian person. The body types are completely are so different and when I first came to Korea, I was amazed at the low weight of local women for their heigh which would put them as underweight yet they looked normal or even chubby. It most certainly is not a one size fits all tool.
How did you come to think and blog about this? Was there anything that inspired you in particular to write about BMI?
Used as one tool within a range of others is a good idea, as well as adjusting it. I think that too, or at the very least making it clear that it’s not accurate because it doesn’t account for various variables and other factors. The BMI result as-is shouldn’t be so heavily implemented or replied upon because it’s not the whole story. Very good point about ethnicity and weight, so thank you for sharing that. You’re so right, it’s “the norm” for smaller sizes for the Asian population, but in the UK/US it’s considered underweight or very slim, unless of course you’re a model (in which case it’s probably still overweight!)
Good question about what prompted me to write about it. Two things, I guess. One is that it’s often referred to in my life by medical professionals and even within my legal case against a surgeon, and it’s used almost in an accusatory fashion. “Your BMI is too low”, as though it’s my fault and it’s an awful thing. But if you look at my thighs, you’d think I was a “normal” weight, and I feel like an okay weight in myself now after gaining some. They also never consider that BMI doesn’t account for my osteopenia (likely osteoporosis by now), loss of muscle mass or that my large bowel was stolen. If I had greater bone density, some muscles and a large bowel I’d probably be nicely in the “healthy” range. The second thing was seeing yet another story of a parent’s anger after their happy and healthy-looking 10 year old child was deemed overweight after his class had their routine BMI checks done. Kids have enough to contend with and so many, boys as well as girls, develop confidence issues, unhealthy relationships with food, body dysmorphia, eating disorders and so on. They don’t need the inaccuracies of BMI giving them another reason to feel unsure in their own skin.
Thanks for your great comment lovely! I hope the week is treating you well so far (and I’m sorry it has taken me so long to reply!) 💜 xx
Very interesting post Caz! I personally think the BMI index is not accurate enough and should be replaced for another method or be part of another measurement system that take into consideration other very important variables the BMI gives a miss.
Another great article pulling the info together Caz.
The biggest issue where there is a problem is heavier skeletal and not taking into account the muscle mass on some larger people when they in fact do work out and are fit.
It’s tough though. I do like calipers and or under water weighing but they have inaccuracies as well! Nothing is perfect but we need a base. Fat is fat and adipose fat is one thin, intramuscular another. Both need to be addressed. I still use my tried and true tape measure of 50 years and that tells a 1,.000 words.
For now it’s a good tool until something better comes along but a multi level approach is important.
💞
Thank you very much for the comment, Cindy, I’m glad you like the post. You’re right, a bigger “build” and muscle mass, or vice versa, will skew results and while BMI/tape measures/calipers/basic weighing etc are useful, they’re not ideal unless you take a multi-faceted approach. You mentioned under water weighing – is that exactly as it sounds (like weighing yourself while submerged)? I’ve never heard of it being done before but I’m curious! xx
Oona: “I AM SMOL! I NEED TO GET MY BMI UP SO I CAN COMPETE WITH THE BIGGER CATS!!!”
EAT YOUR SPINACH, GROW THE MUSCLE, BE POPEYE!
Our health portal shows your BMI front and center every time you log in and mine shows as slightly overweight. I mentioned this to my wife once and she rolled her eyes at it and mentioned, among other things, about how BMI doesn’t distinguish between fat and muscle. Seems like an overly broad brush to paint with …
Absolutely, a broad brush indeed. And yet it can be heavily relied upon by medical professionals and governments to categorise people. I’m underweight and it doesn’t distinguish that I’ve got no muscle mass left these days 😂 We don’t need a constant reminder as it feels a lot like judgement if the result isn’t “normal”.
Super interesting topic! I remember when COVID vaccines first came out, they were only giving them to people considered high risk (at least here in the States), which included people who are obese. A lot of our professional athletes (who are very lean) qualified as obese, just based on BMI, because – as you pointed out – muscle weighs more than fat. I think that’s a good example of why BMI isn’t a good measure. We all have different bodies with different capabilities, and I think that needs to be taken into account.
Ooo that’s a good point about the criteria for at-risk with Covid. This is why it’s worrying that BMI is too heavily relied upon because it’s used to inform decisions about healthcare when it’s just not accurate. It seems silly it’s still taken at face value in this day and age when it’s quite obviously not able to capture individual variables. Thanks for reading and the great comment, Lindsay! I hope you have a good week ahead 💜 xx
This is a really interesting and thought-provoking post, Caz, as are all your posts. I’m not keen on using BMI to judge whether someone is under or overweight, either. Having been both anorexic (and hospitalised) and a compulsive overeater, I was constantly being told my BMI was either too low or too high. It was never taken into account that I was very small-boned (I have to wear children’s sized watches and rings), and then, in later years, working out in the gym when I had muscle.
Now, I am a healthy weight in my eyes (although I think if I worked out my waist-to-hip ratio, I’d probably be unhealthy), and I don’t worry about my BMI. I definitely think it’s an awful idea to judge children’s weight by BMI tables, especially if they are then told they are over or underweight. It’s the ideal way to give them a ‘complex’ and can lead to eating disorders. Eating disorders are now being diagnosed in young children, which is heartbreaking. I’ve also noticed that restaurants and some cafes now have the calorie content of every menu item. I can imagine how negatively this must affect anyone with eating problems. Even now that I’m well, I find myself making choices based on the calorific content. If it has that effect on me even these days, what is it going to do to more vulnerable people?
One point you made was about people with osteoporosis being lighter because of their bone density – I have very severe osteoporosis and have never thought it could make a difference to my weight. It makes perfect sense now. Bones are heavy, so it goes without saying if you have less bone, you will be lighter. Thanks for making that point.
I’m sorry that I’ve been a bit absent from your blog recently. I’ve been concentrating on going to London (last week) to protest against the government because of their total inaction in dealing with the climate emergency. There were 90,000 people protesting in London that weekend, and it was very peaceful with no trouble. It wasn’t even mentioned in the press or in the media. You can bet if there had been any trouble, it would have made all the headlines! It was a lot of hard work, and it’s left me feeling very tired, so please forgive me if my reply seems a bit squiffy in places 😬. I’m not sure I made much sense. Either way, thank you for raising such an important topic, Caz. I do hope you are as well as you can be. Sending you love and healing hugs Xx 🥰💕
I’m really glad you like the post, thank you! I’m sorry you’ve struggled with EDs, too. BMI, and weight generally, can be very triggering for plenty of people and it’s all taken at face value, without considering the limitations or the individual variables. BMI is also, I’ve found anyway, used in a way that seems very judgemental. You’re right about calories on menus – I think it’s good to have them if you want them, but they should be found by those that want them, like online. Having them for all to see and shoving it in their faces can be dangerous – it not only helps to ruin the meal and limit your choices, it could also give those without calorie counting concerns a reason to start. Calorie counting is something that’s really, really difficult to stop and for some it never really does, the voice in your head just gets a little quieter. All these measures are doing, from making chocolate bars tiny and adding calories to menus, is creating more anxiety.
I’m sorry about your osteoporosis, too. But yes, less dense bones will be a bit lighter. Likewise smaller builds generally like yours and mine will be lighter.
I’m sorry I’ve not been around that much in the blogging world either – look how long it took me to reply to your awesome comment! 😂 I really appreciate you taking the time to write all of this, especially when you’ve been so busy.
The protest you attended – was that walking in the road? I saw that in the news. I get the feeling the media like to show the protests that cause frustration, like blocking roads or damaging property, and they skip over peaceful ones because they don’t create outrage and sell papers. What did you do when you were there? Whatever route you took, I hope you’re happy with how it went and well done for pushing yourself despite your health. I’m not surprised you’re knackered! I hope you’ve had the time you need to rest up a bit and get back to baseline.
Sending lots of love and gentle hugs 🌻 xxxxx
Yes it should be scrapped! There is soooo much wrong with it. As someone who developed an eating disordered and suffered for years with it due to this intense focus on the BMI scale, I feel anxious about my kids being pressured to put all faith in it too. There is so much flawed with it. It’s not a sole indicator of health. Measurements of blood pressure, cholesterol, general fitness etc. a=should all surely be seen as a better indicator?
I’m sorry for what you’ve been through with an ED, too. It really, truly sucks, and for so many there’s no real “getting over it”, it can linger in your life and just get a bit quieter. It worries me a lot that more people will fall into it through the ignorant decisions of our healthcare providers and governments. The focus on obesity, calories on menus, making chocolate bars smaller, etc etc. BMI is one such issue because it’s so often taken at face value, with any result other than “normal” used in a judgemental way. I think with your experience, and your knowledge around health too, you’ll be able to educate your kids and reduce the chance of them putting too much stock into weight, food, how they look, etc. It’s not fool-proof of course, but you can only do what you can do. I agree with that last bit you said on the health side of things because weight itself even doesn’t equal health all the time. You can be overweight and really healthy and fit, so BMI or what the scales say doesn’t have any value whatsoever in judging their healthiness.
I know you guys have had a lot going on lately – please go easy on yourself and I hope the week ahead treats you kindly 💜